Конференция «Лазерная флебология 2018», 24.05.2018г., Санкт-Петербург (Иностранные спикеры)
24 мая 2018 года в Санкт-Петербурге под эгидой «Санкт-Петербургской Ассоциации Флебологов» состоялась научно-практическая конференция с международным участием «Лазерная флебология 2018», которая была посвящена фундаментальным и практическим аспектам применения новых методов лечения во флебологической практике.

Президиум конференции «Лазерная флебология 2018» во главе с профессором Шайдаковым Е.В.
В конференции принимали участие ведущие Российские сосудистые хирурги, флебологи и косметологи. Из приглашенных международных спикеров в форуме приняли участие ведущий бразильский флеболог Kasuo Miyake и хирург-флеболог из Сербии Petar Dragic. Руководитель клиники флебологии «МИФЦ» Семенов Артем Юрьевич принимал непосредственное участие в работе конференции.

Семенов А.Ю. с профессором из Бразилии Казуо Мияки на конференции
Первым сделал сообщения доктор из Бразилии Kasuo Miyake. В своих докладах Kasuo Miyake коснулся темы развития техники CLaCS в Бразилии, рассказал и обосновал свою классификацию эстетических венозных нарушений и показал, как он пользуется во время сеансов крисклеротерапии и криосклеролазера «Дополненной реальностью».

Докладывает доктор Kasuo Miyake (Бразилия)
Kasuo Miyake – член бразильского общества сосудистых хирургов и ангиологов, почетный член аргентинского колледжа хирургии вен и лимфологии, основатель и президент ежегодной международной конференции по эстетической флебологии IMAP (International Meeting on Aesthetic Phlebology), основатель техники CLaCS (Крио-лазер и Крио-склеротерапия).
В своем первом сообщении: «ClaCS: криолазер и криосклеротерапия. Почему и как?» Доктор Kasuo Miyake обратился к истории своей семьи. Изучение побочных эффектов склеротерапии было начато ещё его отцом, Хироши Мияки, в докторской диссертации в Университете Сан-Паулу (1972г.)

Отец Kasuo - Hiroshi Miyake (Бразилия)
«Физиопатология язвенных дефектов при склеротерапии: экспериментальное исследование на кроликах». Животным были выполнены подкожные инъекции в объёме 1 мл нескольких склерозирующих препаратов в область ушных раковин под давлением 300, 500 и 700 мм ртутного столба.
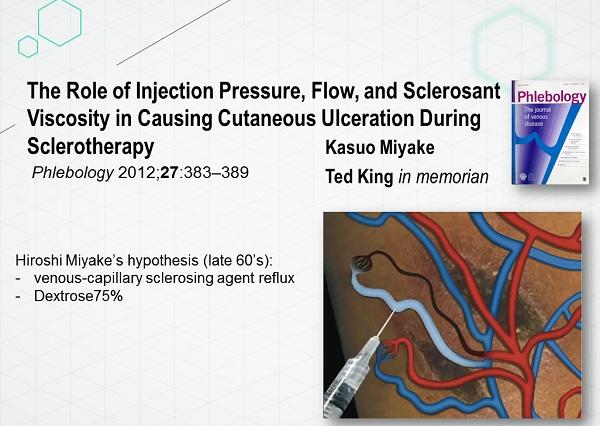
Исследовалась роль давления нагнетания, количество и вязкость склерозанта для получения язвенных дефектов. В последующие годы Хироши Мияки активно практиковал хирургию (микрофлебэктомию) телеангиоэктазий, а в 1989 году активно занимался их лечением путём введения в сосуды 75% раствора глюкозы.
Вторую часть доклада Kasuo Miyake посвятил методике ClaCS. Возникновению этой технологии предшествовали:
- 1995-1999гг. – появление медицинских транскутанных лазеров.
- 1999г. – появление длинноимпульсных лазеров с длиной волны 1064 nm.
- 2000г. – начало использования контактного охлаждения.
- 2003г. – появление специальных охлаждающих приборов.
- 2005г. - исследование устройства Vein Viewer для улучшения визуализации сосудов.
- 2006г. - появление ClaCS крио-лазерная и крио-склеротерапия.
Метод ClaCS, в оригинальной версии, это инъекции склерозирующего 75% раствора глюкозы с последующим воздействием длинноимпульсного лазера с длиной волны 1064 Нм.
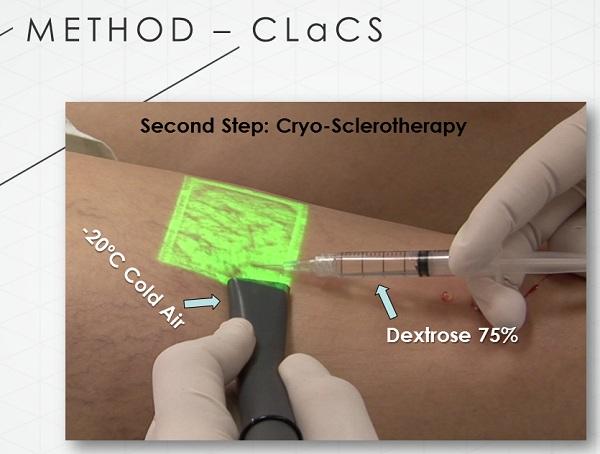
Первый этап CLaCS – инъекция в сосуд 75% раствора глюкозы

Второй этап CLaCS – воздействие на сосуд лазера с длиной волны 1064 Нм
Вся процедура проводится с охлаждением кожи потоком воздуха (-20 ̊ С). 75% раствор глюкозы вызывает осмолярное поражение эндотелия сосудов, лазерное излучение индуцирует термическое поражение как интимы, так и средней оболочки сосуда (tunica media). Воздействие лазера и холода способствуют сужению вены, что, соответственно, уменьшает и внутрисосудистый сгусток крови. Последнее значительно снижает вероятность такого осложнения, как гиперпигментация.
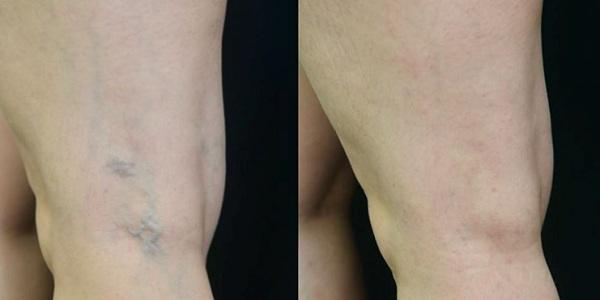
Фото до и после процедуры CLaCS (Kasuo Miyake, Бразилия)
ClaCS проводится в клинике Miyake с 1999 года с фото документацией всех процедур. Доктор Kasuo Miyake выделил следующие достоинства метода:
- Возможность отказаться от применения компрессии.
- Воздействие прямых солнечных лучей допустимо на следующий день после процедуры.
- Полное отсутствие таких осложнений, как: некроз кожи, тромбоз глубоких вен и эмболия, анафилактический шок и смерть.
- Гиперпигментация кожи имела место только у 0,67% пациентов, а ожоги кожи - у 0,11 %, что существенно ниже, чем при изолированном применении классической склеротерапии или транскутанного лазера.
Petar Dragic сделал два доклада: «Лазерная кроссэктомия – риск или надежность? » и «Три года применения методики криолазерной склеротерапии».

Докладывает хирург-флеболог Petar Dragic (Сербия)
Петер Драгич, известный европейский флеболог из города Сомбор (Сербия), основатель клиники «Dr Dragic» в городе Белград (Сербия) и городе Баня-Лука (Босния и Герцеговина). Своё первое сообщение Петер посвятил теме «Преимущества ClaCS. Криолазер и криосклеротерапия.»
Доктор Драгич поведал об истории своей клиники - «Dr Dragic», которая была основана в городе Нови Сад (Сербия) в 2007 году. В последующем открылись филиалы в Белграде (Сербия) и Бане-Луке (Босния и Герцеговина). Клиники отличает высокая специализация и эстетическая ориентированность.

В клинике флебологии «Dr Dragic» (Сербия)
Клиника «Dr Dragic» первой в регионе начала практиковать эндовазальное лазерное лечение, а ClaCS-терапию - первой в Европе (в 2015 году). В настоящее время в клинике функционирует образовательный центр при поддержке и протекции Biolitec и Covidien. На данной образовательной базе уже прошли обучение более 100 специалистов из различных регионов Европы. Центр флебологии «Dr Dragic» специализируется на лазерной хирурги вен и ClaCS-терапии, где ежегодно выполняется более 1000 процедур.
В продолжение сообщения Доктор Драгич обратился к технологии ClaCS. Процедура состоит из:
- Чрескожного лазерного воздействия.
- Воздушного охлаждения (до -20 ̊ С).
- Микроинъекций раствора глюкозы.
- Визуализации при помощи веновизора.
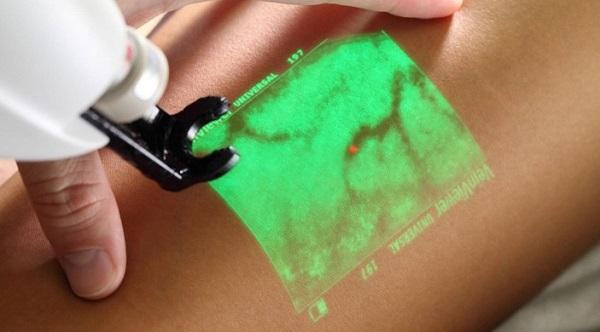
Использование Vein Viewer для улучшения визуализации сосудов
Все компоненты данного метода являются абсолютно натуральными, что снижает вероятность аллергических реакций и прочих побочных эффектов. Единственными аллергенами являются фотоны, охлаждённый комнатный воздух и раствор глюкозы. Это позволяет снизить частоту таких осложнений, как:
- Аллергические реакции.
- Гиперпигментации.
- Полностью избежать появления некроза и язвы.
Доктор Драгич назвал причины эффективности метода:
- Сочетание воздействия склеротерапии, лазера и охлаждения даёт лучшие результаты.
- Удаление питающих вен становится залогом длительного безрецидивного периода.
- Процедура позволяет удалять не только телеангиоэктазы и ретикулярные вены, но и вены, которые не определяются невооружённым глазом, расположенные на глубине до 1 см.
- Позволяет эффективно удалять сосуды в таких непростых зонах, как голеностопный сустав и стопа.
Второе сообщение доктора Петера Драгича было посвящено лазерной кроссэктомии. В клинике «Dr Dragic» было проведено исследование пролабирования сгустка крови в просвет бедренной вены (наличие EHIT) при лазерной облитерации ствола большой подкожной вены.
Позиционирование кончика световода от СФС при лазерной кроссэктомии
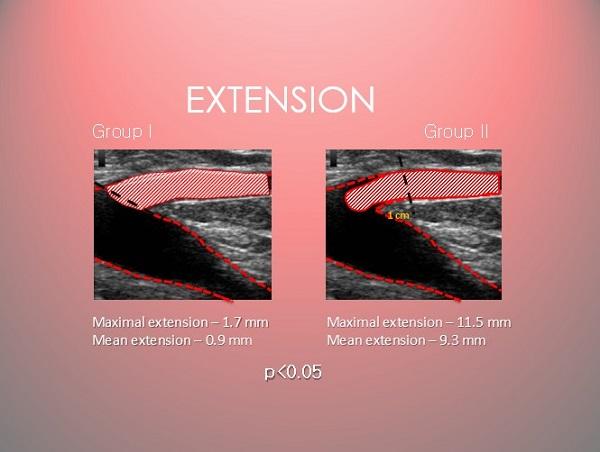
В работу были включены 100 нижних конечностей (50 основная и 50 – контрольная группа) с диаметром в сафено-феморальном соустье (СФС) около 1 см. В первой группе лазерный световод позиционировался в 0,9 мм от соустья, во второй – в 9,3 мм. Результаты:
- В обеих группах среднее пролабирование сгустка составило 0,9 мм.
- При позиционировании световода в 0,9 мм от СФС была достигнута ретракция (сокращение соустья) на 30%, чего во второй группе не наблюдалось.
- Более плотная фиксация сгустка в просвете вены была в первой группе, что теоретически препятствует нарастанию EHIT.
Были сделаны следующие выводы:
- Протрузия сгустка в просвет бедренной вены во время процедуры EVLA (радиальное волокно) на большой подкожной вене диаметром ≤ 1см не связана с уровнем позиционирования лазерного катетера.
- Расширение сгустка крови с образованием EHIT более существенно зависит от характеристик кровотока перед кончиком волокна, чем от уровня позиционирования катетера в просвете большой подкожной вены.
- Расширение и не прилипание сгустка крови во второй группе (позиционирование 9,3 мм от соустья) могут быть предикторами развития EHIT, но для подтверждения этого требуются дальнейшие исследования.
Выступление Российских спикеров в следующем выпуске новостей.
 Чистые Пруды
Чистые Пруды
